Our Position
To ensure continued access to vital physician and surgical services for Medicare patients, Congress must create a fair, long-term, and sustainable solution for Medicare physician payment rates. Lawmakers must take action to improve the physician payment system by providing an inflationary payment update, revisiting budget-neutrality requirements, and maintaining the 10- and 90-day global surgery payment package.

Background
For more than 20 years, physician services have been perennial targets for cuts among lawmakers and as a result, the Medicare payment system has failed to keep up with inflation. In fact, from 2001 to 2023, Medicare payment for physician services have been effectively cut by 26% when adjusted for inflation, and in 2023 physician services were subject to another 2% cut after the passage of a scheduled cut to the Medicare payment program. This continued targeting of payment for physician services creates financial instability for independent practices and consequently, endangers access to care for Medicare beneficiaries.
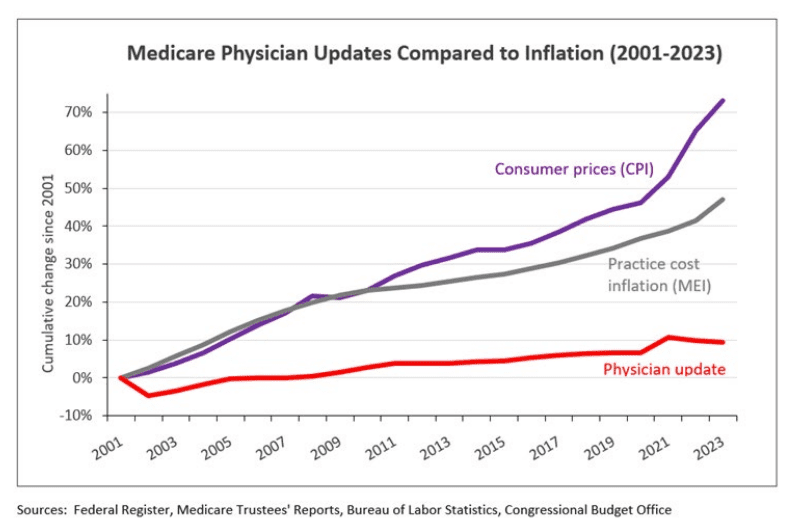
Recognizing the need to act, in March 2023, the Medicare Payment Advisory Commission (MedPAC), an independent, nonpartisan agency providing Congress with analysis on the Medicare program, recommended for the first time that Congress tie physician service payments to the Medicare Economic Index — a measure of inflation pertaining to medical practice costs. This action is an important first step in recognizing the deficiencies in the Medicare program and implementing modifications to make the program work better for physicians and patients.
Congress must ensure fair Medicare reimbursement for physicians
In order to protect access to care for Medicare patients and ensure stability for physician practices, the Academy asks members of Congress to endorse the Strengthening Medicare for Patients and Providers Act (H.R. 2474) to tie Medicare payments to the Medicare Economic Index.
Resources
- AAO-HNS One-Pager on Medicare Reimbursement
- March 15, 2023 Coalition Letter to Congress Recommending Inflation-Based Payment Update
- 🚨 Call to Action: Contact Your Representative to Support the Strengthening Medicare for Patients and Providers Act (H.R. 2474)
- October 28, 2022 AAO-HNS Letter in Response to MACRA RFI
